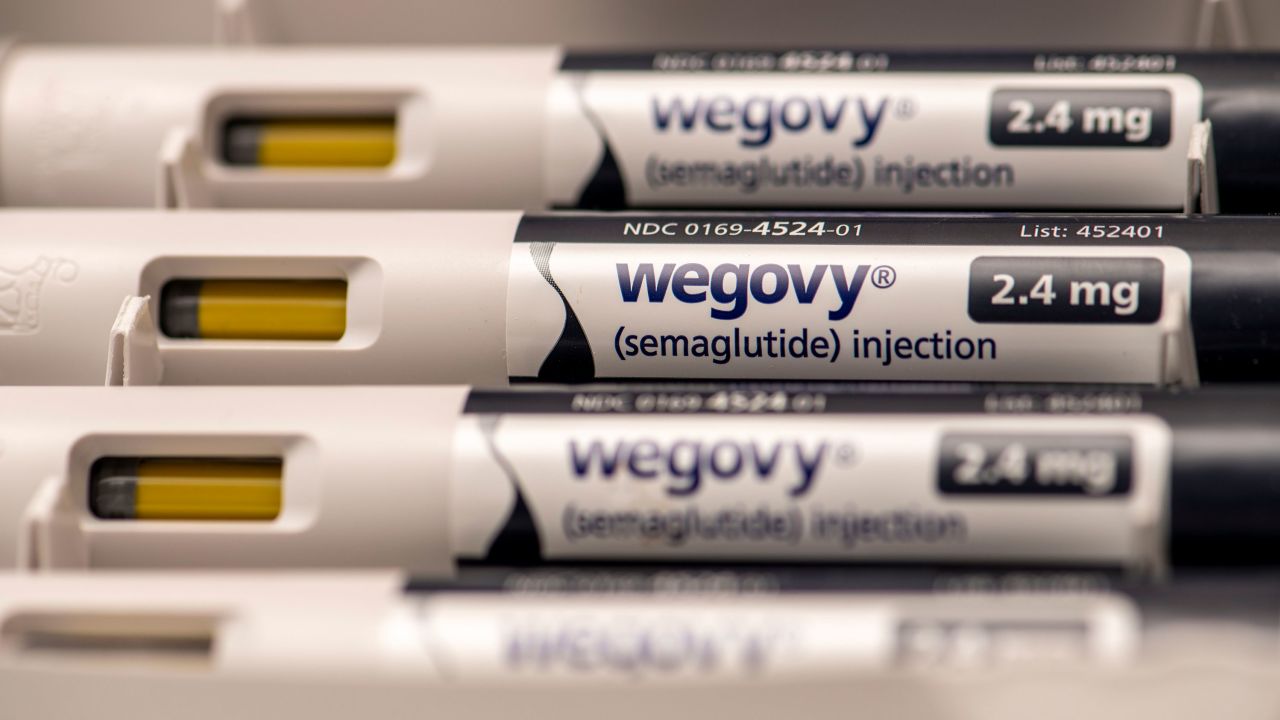
Results from a landmark clinical trial this summer suggested, for the first time, that a medication given for weight loss alone could reduce the risk of heart attack, stroke or heart-related death in people with cardiovascular disease, bolstering physicians’ excitement about an already-exploding class of new medicines.
Novo Nordisk’s Wegovy, part of the booming group of drugs called GLP-1 receptor agonists, was shown to reduce those people’s risk of another cardiovascular event by 20%, results that were confirmed in a presentation of the full dataset Saturday at the American Heart Association conference in Philadelphia.
“Imagine a future where we’re treating obesity and, in effect, treating these other obesity-related diseases” like hypertension, high cholesterol and type 2 diabetes, Dr. Ania Jastreboff, director of the Yale Obesity Research Center, who helped conduct the trial, said at a briefing Friday. “Treating obesity clearly improves health outcomes.”
A key question about the initial results, though, remained not fully answered: Is the heart benefit from Wegovy attributable to how much weight people lose while using the medicine? Or is it because Wegovy has other effects as well?
“It remains unclear to what degree the trial findings were dependent on weight loss, concomitant reductions in risk factors, or other salutary mechanisms of GLP-1 receptor agonism,” Dr. Amit Khera, of the University of Texas Southwestern Medical Center Dallas, and the National Institutes of Health’s Dr. Tiffany M. Powell-Wiley wrote in an editorial that was published Saturday in the New England Journal of Medicine along with the full results of the study, called Select.
Nonetheless, they added, “We are in a new era of treating obesity and cardiometabolic risk with a growing armamentarium of options.”
The tool chest grew this week with US Food and Drug Administration approval of Zepbound for obesity, a drug from Eli Lilly that will compete directly with Wegovy.
Both medicines were preceded by drugs for type 2 diabetes that use the same active compounds: Wegovy’s sister drug is Ozempic, and both use semaglutide, while Zepbound’s is Mounjaro, and both use tirzepatide. They’re all taken once a week as a self-administered shot.
GLP-1 receptor agonists mimic hormones that stimulate the production of insulin, promote feelings of fullness and reduce appetite. Semaglutide targets GLP-1, while tirzepatide targets both GLP-1 and a hormone called GIP.
The trial showed that after two years, people using Wegovy were less likely to develop diabetes or blood sugar levels considered “prediabetes”; lost 9.4% of their body weight, compared with 0.9% on placebo; reduced their waist circumference by an additional 6.6 centimeters over placebo; and had greater reductions in systolic blood pressure, a marker of inflammation called C-reactive protein and triglycerides.
To cardiologist Dr. Steven Nissen of the Cleveland Clinic, who wasn’t involved in the trial but is leading a similar one of tirzepatide, those effects are all evidence of the benefits of weight loss.
“When you lose weight, a lot of things change,” Nissen said in an interview Saturday from the conference just after the Wegovy study presentation, which was given to a packed house with several rows of audience members standing at the back.
“We now have, for the first time in history, treatments that can actually really [help patients] lose enough weight to make a difference,” Nissen said.
Tirzepatide has shown greater levels of weight loss than semaglutide in clinical trials, leading many, including Nissen, to hope it will show even stronger cardiovascular benefits.
The Wegovy study, sponsored by Novo Nordisk, enrolled 17,604 people whose body mass index was 27 or higher, putting them in the overweight category, and who had cardiovascular disease, meaning a previous heart attack or stroke or symptoms of peripheral artery disease – clogged arteries in the arms or legs.
Importantly, participants didn’t have a history of diabetes; a previous trial had shown that treating people with diabetes with a GLP-1 drug, Ozempic, reduced their cardiovascular risk.
The Wegovy trial showed that 569 of 8,803 people taking the drug had a heart attack or stroke or died from heart-related causes, or 6.5%. That’s compared with 701 of 8,801 people on a placebo, or 8%. The difference in those rates is what amounts to the 20% benefit reported in August.
The benefit was seen on top of medicines like statins to lower cholesterol, which 90% of the trial participants were taking, and other drugs considered the standard of care for heart patients.
“The differences in rates between the two treatment groups began to emerge very early after initiation of treatment, within the first months,” the Cleveland Clinic’s Dr. A. Michael Lincoff, who led the trial, said Friday.
The 20% reduction was on a combination of three measures; when looked at separately, not all reached statistical significance. The first individual measure the researchers looked at was death from cardiovascular causes, and while it appeared Wegovy lowered the risk by 15%, the results weren’t statistically significant, meaning they don’t hold as much weight.
The biggest benefit appeared to be in preventing heart attacks, where the risk reduction was 28%. Strokes were reduced by 7%. It’s unclear what the statistical significance of those measures was, because researchers didn’t calculate those values after the finding on deaths didn’t meet the threshold. The overall finding of 20% risk reduction, though, was statistically very strong.
The study didn’t uncover any new safety concerns, but it found that more people stopped taking semaglutide than placebo because of adverse events. The most common were gastrointestinal disorders like nausea, vomiting and diarrhea, and there was a small increase in gallbladder-related disorders on Wegovy compared with placebo.
The amount of weight loss seen in the trial, 9.4%, was less than in other studies of Wegovy, which showed average weight loss closer to 15%. Lincoff noted that this trial wasn’t focused on weight management, where trials typically involve changes in diet and exercise and “close monitoring,” but instead “models the way cardiovascular disease is treated in the real world.”
He also noted that not all of the participants got the highest dose of Wegovy in this study; the dose of medicine was adjusted based on whether they had side effects.
On the question of whether the benefit in the trial came primarily from weight loss or from other drug effects, Lincoff pointed out that the heart benefits became apparent in the study earlier than the major differences between Wegovy and placebo on weight loss, and he noted that “lighter-weight patients to start with experienced the same magnitude of benefit.”
“I think most of us believe that some of this is weight loss, but I think that that oversimplifies a very complex molecule, a complex receptor on multiple tissues, and I don’t think it’s as a simple as that,” he said. “That’s part of the reason why I don’t think weight loss itself is the surrogate; we have to look at the mechanism of the weight loss.”
“And,” Jastreboff added, “it may be a combination of both.”
Get CNN Health's weekly newsletter
Sign up here to get The Results Are In with Dr. Sanjay Gupta every Tuesday from the CNN Health team.
The study left a few additional questions unanswered: It looked at heart risk only in people with existing cardiovascular disease, and researchers said it would be important to know whether the drug could benefit people who hadn’t had a cardiac event. The trial also had racial and gender imbalances: Only 3.8% of participants overall were Black, and 28% were women.
The findings are expected to increase demand for the drug, which already is in short supply, and potentially improve insurance coverage, which is spotty. Wegovy costs $1,349 a month before insurance.
And while “millions of additional patients” could benefit from the drug based on these results, Khera and Powell-Wiley wrote in their editorial, “semaglutide comes with a significant cost both to patients and to society at the current pricing for GLP-1 receptor agonists, which makes this treatment inaccessible for many.”